- Diabetes can damage tiny blood vessels in your eyes, affecting your sight.
- If this does happen, quick treatment can help preserve your vision. It’s important to get in touch with your eye doctor right away if you notice anything.
- Lifestyle changes can help to steady your blood glucose levels, protecting your sight.
Vision is so key to our experiences. If you have diabetes, taking care of your eyes becomes especially important. You are at higher risk of developing diabetic retinopathy, a complication of diabetes that affects the eyes. A third of people diagnosed with diabetes have this condition. Although diabetes is a leading cause of blindness, you can protect your vision with proper eye screening and treatment.
Diabetes and your health
Diabetes affects the entire body. Body cells require glucose to survive. Normally, the amount of glucose (sugar) in the blood is tightly controlled. The pancreas keeps blood glucose levels within normal range. When these levels rise after a meal, the pancreas makes a hormone called insulin. Insulin signals the body cells to take up glucose from the blood. Insulin’s job is to remove glucose from the blood to prevent damage to the organs.
In diabetes, the body doesn’t make enough insulin or use what is made effectively. Too much or too little glucose in the blood can disturb how the body’s organs function.
How does diabetes affect vision?
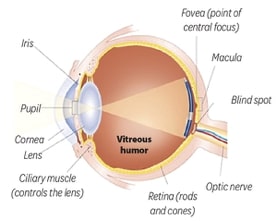
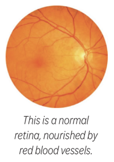
Diabetes damages the blood vessels that nourish the retina. The retina is a sensory layer at the back of the eye. It changes images passing through the pupil and lens into electric signals. These signals are sent through the optic nerve to the brain.
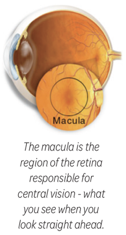
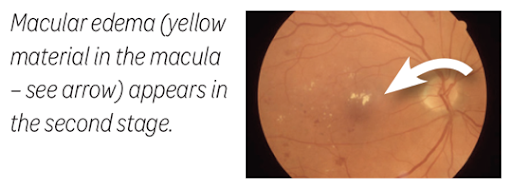
One part of the retina, called the macula, is especially sensitive to light and provides central vision. When you read or look at an object, your macula allows you to identify details and detect small changes in colour and texture.
Many small blood vessels supply the cells of the retina with blood. The blood vessels provide oxygen and nutrients to the cells, and drain waste products. Unless the cells receive a constant supply of nutrients and oxygen, they cannot do their job well. When this happens, your sight can be affected.
When diabetes is poorly controlled, the blood vessels feeding the retina can become leaky. Fluid can seep into the retina (and macula), causing it to swell. Swelling in the macula disturbs central vision. Since the retina is not getting enough nutrition, abnormal blood vessels begin to form. These new blood vessels are fragile and can bleed inside the eye, causing floaters and vision loss.
Stages of diabetic retinopathy
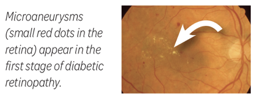
Mild non-proliferative diabetic retinopathy
This stage involves microaneurysms, where the blood vessel wall swells out to form a balloon-like pouch. Microaneurysms can affect the flow of blood through the blood vessel. At this stage, vision may not be noticeably affected, but the problem becomes more severe with time if not treated.
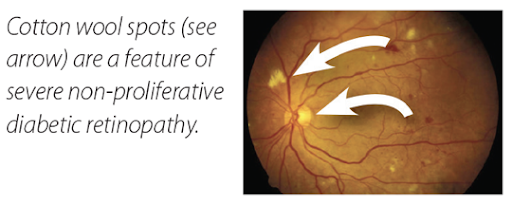
Severe non-proliferative diabetic retinopathy
As more and more blood vessels are blocked, larger regions of the retina lose their supply of nutrients and oxygen. More bleeding can be seen in the retina. Patches of retina without enough blood begin to die and appear as white fluffy areas called ‘cotton wool spots.’ Macular edema continues to worsen, and central vision blurs.
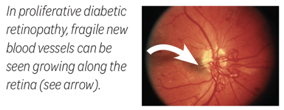
Proliferative diabetic retinopathy and complications
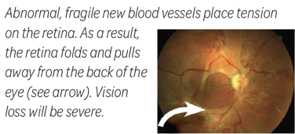
This is the most advanced stage of the disease. Large areas of the retina are not getting enough blood, and new abnormal blood vessels form. These new vessels are fragile and leaky. If the vessels begin to bleed, they can cause severe loss of vision or even blindness. They may also put tension on the retina, causing it to tear and detach (pull off) from the back of the eye.
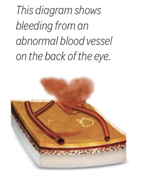
Vitreous hemorrhage
The vitreous is the fluid that fills the large chamber at the back of the eye. When new blood vessels form, they can bleed into the vitreous. Sometimes they only bleed a little, so you might see a few dark spots or floaters.
When they bleed a large amount into the vitreous fluid, the blood blocks all vision. A vitreous hemorrhage can resolve on its own with time. However, any loss of vision may signal serious disease.
If you experience vision loss, visit your doctor as soon as possible.
Traction retinal detachment
If not treated by an ophthalmologist (eye specialist), these new emerging blood vessels can create scar tissue. When the scar tissue shrinks, it can apply pressure to the retina and pull it off the back of the eye. If the retina detaches, you might notice:
- new floaters or flashing lights
- blank or blurred areas in your vision
- a missing section like a curtain in one eye.
Left untreated, complete vision loss can occur. Testing each eye by covering the opposite eye can help you to identify missing areas of your vision.
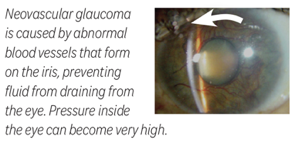
Neovascular glaucoma
Fluid is produced by the eye and drains near the iris (the coloured part of the eye). In proliferative diabetic retinopathy, abnormal blood vessels growing on the iris block fluid from draining. As a result, the pressure inside the eye can increase.
It can damage the optic nerve, lead to intense eye pain and nausea, and severely affect vision. This condition, called neovascular glaucoma, is a serious complication of diabetic retinopathy.
Treatment for diabetic retinopathy
Prevention
While there is no cure for diabetic retinopathy, it is preventable. Lifestyle changes can help you improve blood glucose control.
Diabetes medications or insulin are often needed to help control blood glucose levels, and must be used as prescribed.
Regular eye care
If you have diabetic retinopathy, regular eye examinations by an ophthalmologist are necessary. Monitoring the health of your eyes assesses whether treatment is required. Ophthalmologists can offer treatments for diabetic retinopathy that prevent further loss of vision.
Mild, non-proliferative diabetic retinopathy may not require treatment immediately. Your ophthalmologist will regularly monitor your eyes for changes. If swelling is found in the retina and macula, or if new blood vessels begin to form in the retina, quick action is needed. Without rapid treatment, you may lose your vision.
-
Protect the health of your eyes
- Eat a balanced diet, paying careful attention to the sugar content and glycemic index of foods.
- Regular exercise helps maintain healthy blood glucose levels.
- Quit smoking and manage blood pressure to protect your eye health.
Types of treatments
Treatment for diabetic retinopathy is highly effective. With timely and appropriate treatment, those with proliferative diabetic retinopathy have less than a five per cent chance of becoming blind within five years.
Injections of medications inside the eye can treat swelling of the retina and prevent abnormal blood vessels from growing. Your ophthalmologist will discuss the different medications that can be used. Some people only need an injection once every few months, while others require more frequent injections. Only a specialist should perform injections into the eye. Ask about the risks and benefits of these procedures.
Laser photocoagulation is a common treatment for diabetic retinopathy. An ophthalmologist uses a laser to reduce swelling of the retina or reduce the growth of abnormal blood vessels. Again, these procedures should only be done by a specialist.
With more advanced diabetic retinopathy, such as bleeding inside the eye or detached retina, surgical treatments are offered. Many people, including those with diabetes, require surgery to remove the cataracts that develop with aging. Neovascular glaucoma may also require treatment with eye drops, injections inside the eye, laser treatment, or surgery. Your ophthalmologist can discuss these treatments.

Pregnancy and diabetic retinopathy
Pregnancy can make diabetic retinopathy worse. Keeping blood glucose levels within target range is important. Regular eye examinations are also needed to monitor the health of your retinas and prevent vision loss. If you have diabetes, ask your care team about how diet, lifestyle, and medication use can support your pregnancy.
What if I have already lost some vision?
Talk to your eye care professional. Ask about the major causes of your vision loss, and whether any therapies or surgeries might improve your vision. A wide variety of tools and devices can help to make the most of remaining vision and increase your quality of life.
If you have trouble reading your prescription labels, ask your pharmacist if ScripTalk is right for you. This free app is available at no charge on Apple or Google Play. A ScripTalk station reader can also be loaned to you at no cost as part of the En-Vision America’s Pharmacy Freedom Program. Your pharmacist will program and attach a small electronic tag to your prescription container. When you place the container on your ScripTalk station reader or phone, it speaks the information on the label aloud.
Community health centres, counsellors, Diabetes Canada (→diabetes.ca) and occupational therapists have information about low-vision counselling, training, and special services for people with impaired vision.
Can I tell that my vision is changing?
When you are first diagnosed with diabetes, you may not have noticed any changes to your vision. Diabetic retinopathy may be seen right away, or can take years to develop. You may not know that you have this complication. Your vision may seem normal, even though harmful changes are taking place in the retina. Regular eye examinations by an ophthalmologist can identify diabetic retinopathy and reduce the risk of vision loss.
Blood glucose control – the glycosylated hemoglobin A1C test (HbA1C)
Your doctor can use an A1c test to find out how well your blood glucose levels are controlled. A1c should be measured about every three months. The test requires a sample of your blood.
Glucose in the blood binds to hemoglobin, a protein found in red blood cells.The glycosylated hemoglobin A1c test is a good measure of your average blood glucose level for the two to three-month period before the test is taken.
People with normal blood glucose control usually have a glycosylated hemoglobin A1c of less than six per cent. If you have diabetes, discuss your target HbA1c level with your doctor.
A1c testing may be available** at your Sobeys Pharmacy, Lawtons Drugs, Safeway Pharmacy, FreshCo Pharmacy, Foodland Pharmacy or Thrifty Food Pharmacy. Speak with your pharmacist to learn more.
Save time booking and waiting for lab test results by visiting us in-store to receive your results in minutes and get any necessary recommendations for your diabetes management**.
**Services not available in Saskatchewan and Manitoba.
How can I protect my sight?
Take an active role in controlling your diabetes. Being responsible for your health and attentive to changes helps prevent complications and vision loss. Protect your vision in the following ways.
- Be alert to changes in your vision, and seek regular eye care. At least once a year, have a dilated eye exam. More frequent examinations are needed for people with severe diabetic retinopathy. During these examinations, drops are placed in your eyes that will make your vision blurry for a short amount of time. Without these drops, a complete examination of your retina cannot be done.
- Report any changes in your vision to your ophthalmologist right away. Get the care you need promptly, as it is a critical part of keeping your eyes healthy. Be on the lookout for blurry or hazy vision that lasts more than a few hours. If you notice sudden floaters (black spots in your vision), contact your ophthalmologist.
- Monitor and control your blood glucose levels. Ensuring that your blood glucose is tightly controlled slows damage to your retina and prevents severe loss of vision over time. Since your body’s glucose response system is not working properly, you must keep your glucose levels as normal as possible. Frequent blood glucose testing and regular follow-up with your family doctor or internist will help you to achieve the best possible glucose control.
- Control your blood pressure.
- Reduce your cholesterol level if it is too high.
- Stop smoking. Smoking can increase your blood pressure as well as your risk of heart attack, stroke, cancer, and lung disease. Talk to your doctor or pharmacist about ways to quit smoking.
- Reduce stress. Stress causes rapid swings in blood glucose levels. Under stressful conditions, certain hormones are released that cause large changes in blood glucose levels.
A counsellor or support group can help. Use tools like meditation, massage, exercise, and art to reduce stress and increase your overall quality of life.
Talk to your health care team about controlling your diabetes and slowing the progress of diabetic retinopathy. Being actively involved in your health makes all the difference.
WRITTEN BY: Imran Jivraj, BSc, MD, FRCSC, an ophthalmologist, and Matthew Tennant, BA, MD, FRCSC, a retina specialist with Alberta Retina Consultants in Edmonton.

