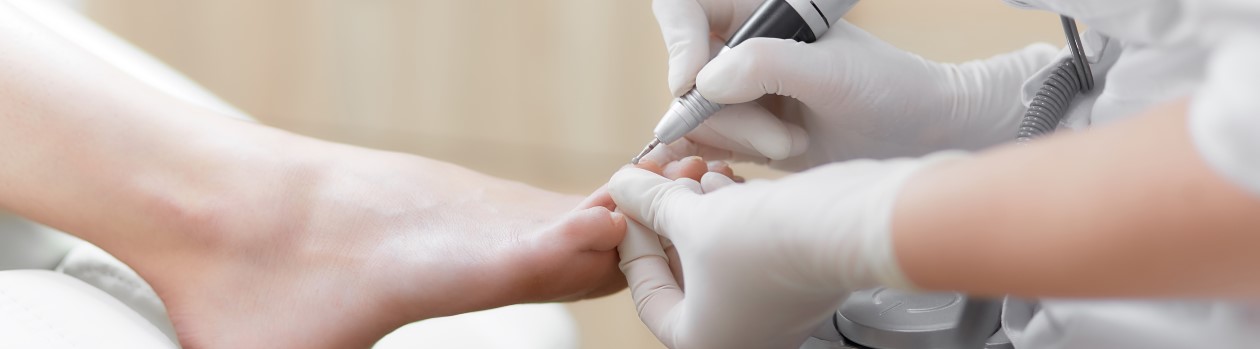
- Be aware of what’s happening with your feet. Numbness and tingling can be a first sign of blood vessel and nerve damage.
- Pedicures are possible, as long as you and your feet are in good health and free of complications. Check our list of questions to ask to make sure the spa or salon can meet specific health standards.
- Clean white socks can be an important part of your daily diabetes foot care routine. If you do have oozing from a cut or sore, you’ll be able to see it.
Our feet are amazing and intricate parts of our bodies that require special attention. While the eyes may be the windows to the soul, the feet support all that we do and deserve particular care. If diabetes is part of your life, diabetes foot care becomes especially important. This chronic condition can cause blood vessel and nerve damage. A warning sign of this is numbness and tingling in the feet. If diabetes remains uncontrolled and the symptoms of numbness and tingling are not addressed, then feeling in the feet may be lost. This loss of sensation can mean that a foot injury goes unnoticed, which could lead to an infection.
Those who have diabetes are 15 times more likely to develop a foot ulcer sometime in their life. According to Diabetes Canada, adults with diabetes have a 20-fold greater likelihood than adults without it of being hospitalized for a lower limb amputation that is not related to trauma, such as a car crash. With these statistics in mind, it is clear that taking good care of your feet is a priority.
Watch for these warning signs when checking your feet
- changes in skin colour, such as redness
- changes in temperature, such as skin that feels hot
- swelling in the foot or ankle
- pain in the legs
- cuts or sores that are not healing or have discharge
- blisters
- corns or calluses – spots of rough skin caused by rubbing or pressure on the same spot
- plantar warts – flesh-coloured growths on the bottom of the feet
- ingrown toenails with the edge of your nail growing into your skin
- toenails infected with fungus
- dry cracks in the skin, especially around the heel
- unusual or lasting foot odor
Diabetes conditions that affect the feet
Diabetic neuropathy is uncontrolled blood glucose causing nerve damage, leading to numbness and tingling in the feet. If the nerves in your legs and feet have been damaged, you may not feel heat, cold, pain or even pressure from ill-fitting shoes. An unnoticed cut or sore on your foot could get worse and become infected, leading to a more serious complication.
Peripheral vascular disease is uncontrolled blood glucose affecting the flow of blood through the body, especially in the legs and feet. Without good blood flow, it takes longer for a sore or cut to heal. An infection that will not heal because of poor blood flow puts you at risk of developing ulcers (open wounds or sores) or gangrene (the death of tissue due to a lack of blood) .For people with diabetes, there is an increased risk which is often more severe and hard to treat.
“The human foot is a masterpiece of engineering and a work of art.”
– Leonardo da Vinci
Other foot problems, such as bunions, corns, calluses, hammertoes, fungal infections, dryness of the skin, and ingrown toenails, may all be related to diabetes. While these problems are not specific to diabetes, nerve and blood flow damage can increase the likelihood of these common complications.
A daily diabetes foot care routine
- First, gather the supplies you need to care for your feet properly. Having everything close at hand can make the routine easier.
- Wash your feet in warm water (not hot). Dry your feet well, especially between the toes. Next, thoroughly check your feet for certain issues using a hand-held mirror. If you still cannot see the sides or the bottom of your foot, have someone check for you.
- Apply a good rich cream or lotion to your heels, especially if they are really dry. You can use the foot file to gently slough off dry skin before applying any cream. However, do not use lotion between the toes as this could promote infection. Old-fashioned petroleum jelly is also a cheap and effective option.
- Finally, put on a pair of fresh, clean white socks every day, along with well-fitting shoes. With a white sock, any drainage from a cut or sore will show through.
If it is difficult for you to see your entire foot, ask your diabetes care team for help. A trained health care provider can cut your nails, file callouses, and give professional advice. While foot care may not be covered by your health plan, consider that avoiding possible issues can be worth the expense. Your healthcare provider can likely provide you with information about reasonably priced clinics in your community.
If you notice a cut, sore, blister, corn or callus, continue to monitor it for a few days. Watch for signs of infection (redness, pain, tenderness, pus, or a foul smell). You may choose to cover the area with a bandage. However, avoid poking or prodding it.
If you notice any signs of infection, see your doctor or go to emergency.
Should you get a pedicure if you have diabetes?
If you and your feet are in good health and free of complications, a pedicure poses very little risk. However, skip the trip if you have neuropathy or any cuts or sores.
Before you use the salon, investigate. Ask very specific questions about sanitization practices, and be sure you get clear answers.
- Foot baths should be cleaned and sanitized after each pedicure.
- Nail tools should be sterilized in an autoclave and placed in a package that is not opened until you are sitting in the chair.
- Avoid salons that use wooden tools or that reuse emery boards. If you choose to bring your own nail tools, make sure you clean them thoroughly when you get home.
Be sure to let your nail technician know that you have diabetes.
Dos and Don’ts for Foot Care
DO
- Trim your toenails straight across and file any sharp edges. Do not cut the nails too short.
- Have your feet measured properly when buying shoes. Footwear should be supportive, and not rub or pinch.
- Buy shoes late in the afternoon. Swelling can make your feet slightly bigger by this time of day.
- Protect your feet by wearing socks and shoes whenever possible.
- Exercise regularly to improve blood flow to your legs and feet. Being active helps keep your blood glucose in target range too.
- Ask your doctor for a referral to a foot care specialist if you have corns (thick skin on toes), calluses (thick skin on the bottom of feet), ingrown toenails, warts or slivers.
DON’T
- Do not cut a corn, callus or wart, or treat it with any over-the-counter products. This can be very dangerous for people with diabetes.
- Stay away from tight socks or tights that may reduce blood flow.
- Do not sit or cross your legs for a long period of time.
- Walking around barefoot is a bad idea, as it increases your chances of stepping on something that can injure your feet.
- If you smoke, please stop. This habit decreases blood circulation and healing, and significantly increases the risk of amputation.
When should you see a doctor?
Your feet should be checked by a health care provider at least once a year to screen for neuropathy and loss of circulation. On every diabetes-related visit, take your socks off to remind your care provider to assess your feet.
See a doctor right away if you have any signs of infection like swelling, redness, warmth or discharge from a sore or cut on your foot. The average healing time for a sore is between three and five days, and it can take as long as seven days for those with diabetes. If you think your sore is healing too slowly, have it checked. A sore should be assessed if it has not begun to heal after a week.
Severe foot complications are usually due to uncontrolled diabetes, or foot issues that are not treated by a health care professional. It may reassure you to know that less than 10 percent of those with diabetes develop severe complications with their feet.
A daily foot care routine, regular foot exams by your diabetes health care team, and prompt attention to any issues that might arise can help your feet to keep supporting all that you do.
For further information, please visit:
Diabetes Canada (diabetes.ca):
WRITTEN BY: Melodee Dayrit, RN, BScN, CDE a certified diabetes nurse educator and clinical nurse leader at St. Paul’s Diabetes Health Centre in Vancouver, BC, with support from her team including Daphne MacDonald RN, BSnN, CDE, Oksana Kunina, RN, BScN, CDE, Tanya Sloan, RN, BScN, CDE and Elizabeth Cabanal, RN, BSCN.